A common complaint and concern is the sudden or chronic appearance of dead skin on your feet.
By understanding the causes and, more importantly, the treatments to deal with these skin conditions, you can ward off even the most uncomfortable and unsightly foot problems.
Dead Skin on Feet
Dealing with dead skin on feet, also known as calluses or corns, happens to the best of us.
Calluses appear on the feet as hard, thickened, dead outer layers of skin.
Calluses are a product of wear and tear, constant pressure, or anything that creates prolonged irritation to the feet.
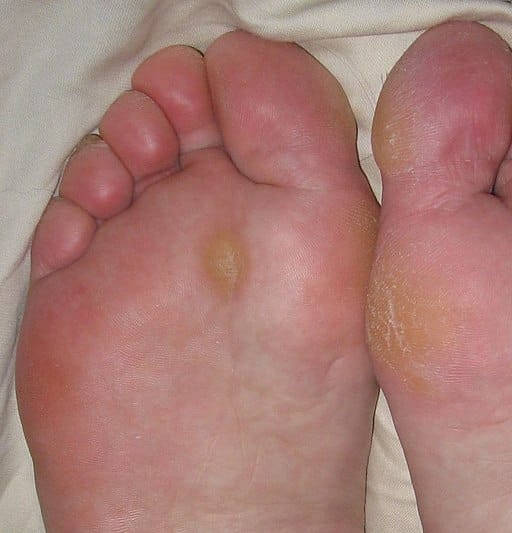
Once your body recognizes that pressure or irritation, calluses form as a means of protection for underlying, healthy skin.
Cell production goes into overdrive, and the outer layer of skin experiences an increase in tissue.
The stimulation of cells and overproduction of tissue cause hard, thick patches of dead skin to form at the outer, protective layer of skin.
Calluses are not typically painful, and other than being thick and hard, they are flat in appearance.
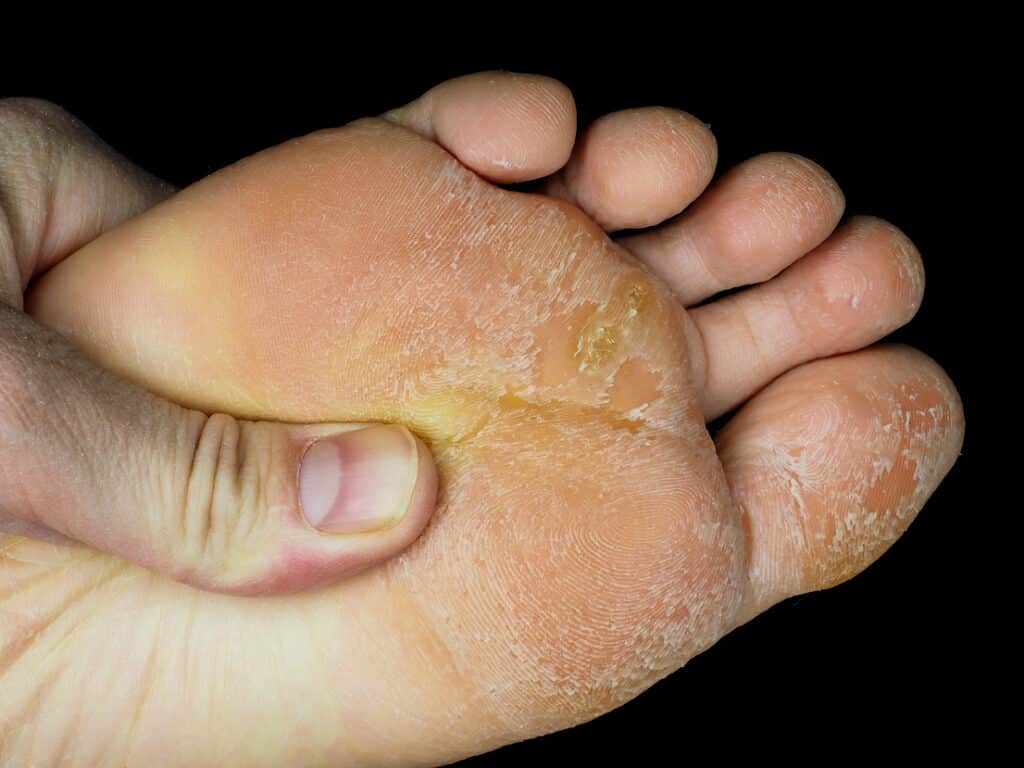
Typical areas of the feet affected by dead skin include the heel, ball, bottom, sides, and especially on the side of the big toe.
A corn is a related affliction, but forms in deeper layers of the skin and is cone-shaped.
They’re painful when pressure is applied.
Dead skin on feet is identified by:
- Hardness
- Thickness
- Dryness
- Dry cracked feet with cuts
- Flaking
- Skin peeling off the bottom of the foot
- Discoloration, or yellowing, of the skin
Causes of Dead Skin on Feet
Dryness, Low Moisture
When your feet are always covered in shoes and socks with no air circulation, they dry out from lack of moisture.

Dry conditions cause the skin to peel, flake, crack, and hard skin on foot keeps coming back.
Soaps
Clean skin is a must when dealing with any type of foot issue.
When cleaning the feet, use a gentle soap to get the job done without stripping the skin from its natural oils.

These harsh or irritating additives can make matters worse by causing rashes, itching, or burning.
Rinse feet thoroughly after washing with even the gentlest of soaps.
Aging
Aging certainly takes a toll on the body, and your feet are no exception.

As we age, dry skin and dead skin on feet become a real and constant issue.
Symptoms of aging feet include excessive dryness, flakiness, the formation of thick/dead skin, circulation issues, and thick, yellow toenails.
Medications – Diuretics
Some medications promote extra dryness to the skin on your feet.
Diuretics dry out the skin because they work to clear water and salt from the body.
While diuretics can lower blood pressure and eliminate excess fluid in the body, but also cause dehydration.
Dehydrated skin dries out very quickly.
Other common medications that cause dry skin on the feet are those used to treat acne, statins for the heart, and antihistamines to fight allergies.
Poor Fitting Shoes
Ill-fitting or tight shoes tend to press toes together for long periods.
Continued use not only causes pain but allows sweat and excessive moisture to attack the feet—extreme moisture results in foot odor and the growth of bacteria and fungus.

Steer clear of tight-fitting shoes, high heels that cram your toes together, and wearing moist socks for extended periods.
Athlete’s Foot
Athlete’s Foot is a dry, cracked foot fungus that spreads to all areas of the feet.
The symptoms of Athlete’s Foot include severe itching, followed by cracking, peeling, blistering, overall irritation/redness, and a scaly appearance.
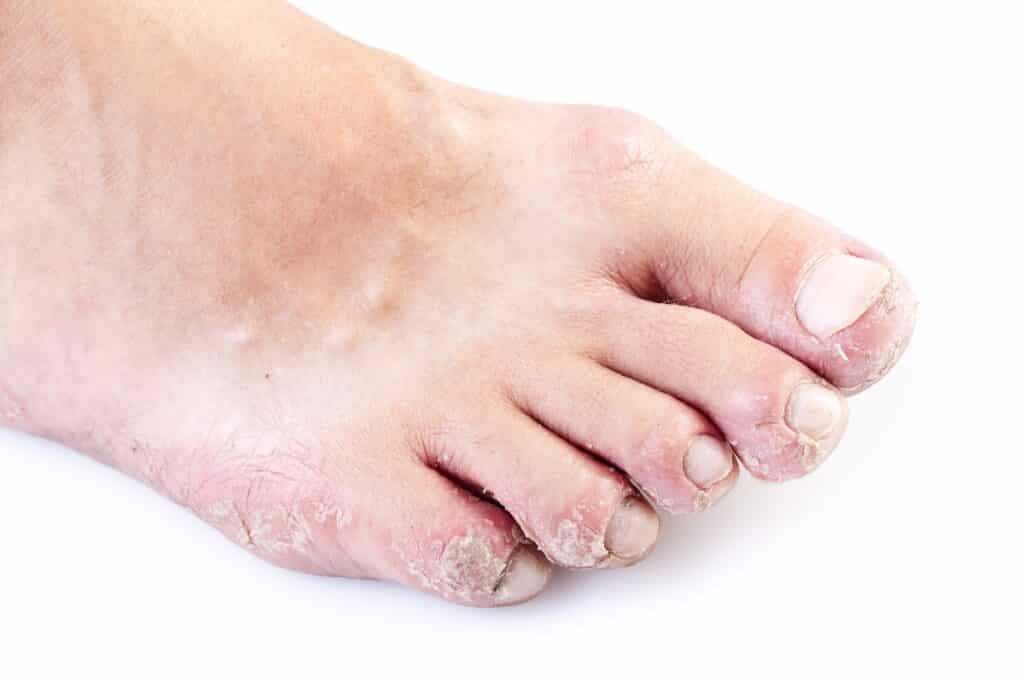
The fungal infection generally starts in between toes when feet are always wet.
While Athlete’s Foot loves dark, moist conditions for fungus to grow and spread, it also attacks dry, flaky skin.
It can also spread to other parts of the body by using contaminated towels, especially after drying off your feet. Athlete’s Foot is not contagious.1Ewa Hrehorów, Joanna Salomon, Lukasz Matusiak, Adam Reich, Jacek C Szepietowski
. Patients with psoriasis feel stigmatized
, Acta Derm Venereol
. 2012
Eczema
There are different types of eczema, and the condition is not exclusive to feet. When it does appear on the feet, it may appear as a typical rash.
The root cause of this affliction is unknown. Still, severely dry skin, exposure to harsh chemicals (like chlorine in a swimming pool), stress, and seasonal allergies may all be contributing factors.
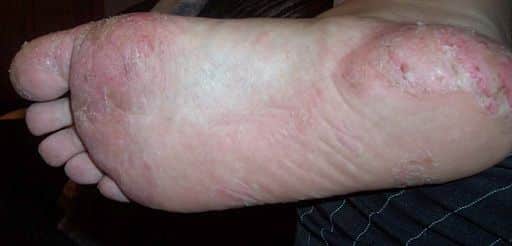
Eczema produces extremely itchy, small blisters, typically on the soles of the feet. By scratching the blisters, they spread.
Eczema is very painful, bleeds and causes dry, cracked feet with cuts in the skin. It may result in the feel and appearance of thick, spongy skin, particularly after scratching the areas.
Eczema affects twice as many women as men2Annette Mollerup, Niels Kren Veien, Jeanne Duus Johansen. An analysis of gender differences in patients with hand eczema – everyday exposures, severity, and consequences
, Contact Dermatitis
. 2014
. Eczema is not contagious.
Psoriasis
Medical professionals believe psoriasis is attributed to genetics or, more than likely, an autoimmune disease.
An autoimmune disease causes the body to turn on itself and attack healthy skin cells.
In the case of psoriasis, cell turnover rate (replacement of dead skin cells with new ones) moves too fast.
Other factors that trigger an outbreak include stress, infection/illness, dry skin, injury/damage to the skin, or a reaction to medications.
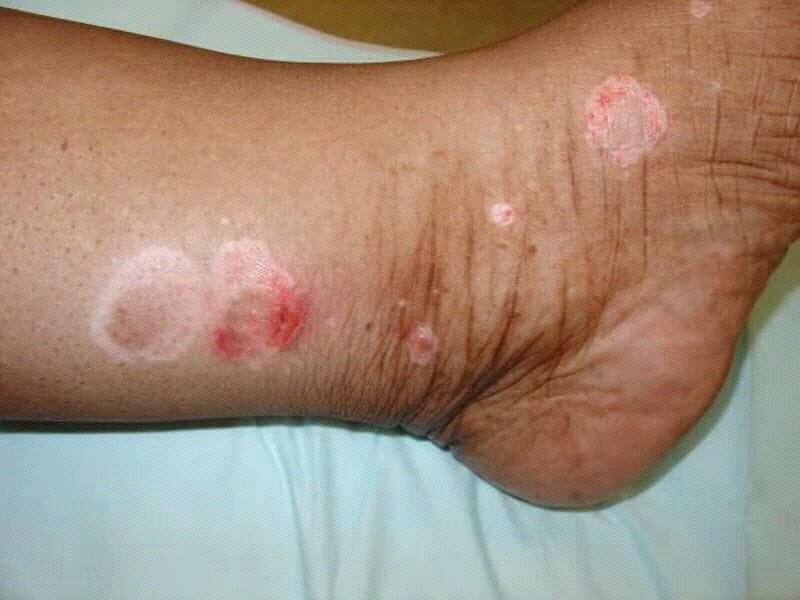
Psoriasis is sometimes confused with a skin infection or Athlete’s Foot because the symptoms are similar.
The symptoms of psoriasis include pain, joint stiffness, toenails that appear swollen and primarily appear on the soles of feet.
In the beginning stages of an outbreak, silver-colored scales appear on the skin.
As it progresses, changes occur in skin color and appearance.
Psoriasis is not contagious.
Diabetes
Because of the high glucose levels that many with diabetes suffer from, body fluid levels are negatively affected.
Due to low body fluid levels, skin tends to be very dry.
The less available fluids, the less you sweat, which also leads to overly dry and dead skin on feet.
Excessive dryness results in flakiness cracked skin and, ultimately, skin peeling off the bottom of the feet.
Diabetic nerve damage in the feet causes the production of natural skin oils to simply stop working, another cause of dry skin.
Hypothyroidism
Hypothyroidism, or an under-active thyroid, causes a higher probability of developing serious, chronic skin afflictions on the feet such as:
- Dry, coarse, rough, cracked skin
- Formation of calluses
- Itchiness
- Poor circulation
- Prone to foot infections
- Foot odor
- Discoloration of the outermost layer of skin on soles of feet
Dryness occurs because sweat glands do not function properly, resulting in poor skin hydration on the feet.
How to Get Rid of Dead Skin on Feet
To understand the causes of skin conditions affecting your feet is one thing.
The goal, however, is to minimize and even prevent them in the first place.
Here are 9 proven ways to remove dead skin on feet:
Electric Callus Remover
An electric callus remover is a handheld device that softens thick, callused skin by exfoliating with a gritty, rotating roller.

The rotating roller spins a full 360 degrees and is extremely effective at tackling any area of the foot where tough, thick dead skin is an issue.
The rollers are available in varying degrees of grit to quickly smooth large calluses or gently buff and soften heels and balls of feet.
For professional results in the privacy in your own home, check out the Electric Callus Remover by Own Harmony.
Exfoliating Foot Scrub
Exfoliating foot scrubs work using alpha-hydroxy acids to soften and lift away dead skin cells.
Exfoliation results in smooth, refreshed skin once the dull, top layer of dead skin is removed.

Massage the foot scrub directly to the skin, concentrating on rough areas.
Work the foot scrub into the foot by hand or use a foot brush to scrub off the dead skin.
Rinse feet thoroughly with warm water to remove all traces of the scrub and pat dry with a clean towel.
Foot Soaks
To soften hard, callused skin, use warm water foot soaks for at least 10 minutes.
Add Epsom salts, essential oils, vinegar, or baking soda for even more of a softening effect.

Foot soaks provide relief from itching and dry, cracked feet with cuts.
Pat feet completely dry after a foot soak. Apply a skin-nourishing cream, lotion, or essential oil before sliding into cotton socks for the night.
Pumice Stone
Soak feet in warm water for at least 5 minutes or until the skin is soft.
Wet the pumice stone while soaking feet as you should never use a dry stone on the skin.

Pat feet dry and rub pumice stone in a gentle, circular motion to soften calluses for about 2-3 minutes, which will remove dead skin on feet.
Foot Files and Foot Graters
Foot files work much like a pumice stone but are handheld devices used to remove dead skin by using a back and forth gliding motion over softened calluses.
Dead skin is removed by gently rubbing away with the sandpaper-like grit on the emery or metal file.

Foot graters are also handheld devices, but instead of using an abrasive sandpaper-like file surface, it looks more like the cheese grater in your kitchen.
Please proceed with caution when using foot graters because it is effortless to remove too much skin and injure the foot.
Taking off too much skin with a metal foot grater results in tearing, bleeding, and pain.
Foot Masks
Foot masks look like booties that slide over your feet.
They work by using natural exfoliating agents.

Apply the mask to clean, dry feet and leave on for about an hour. Remove the mask, wash, thoroughly rinse, and pat dry your feet.
At first, you probably won’t be impressed with the results.
After a few days, the skin will begin to peel. After about a week, the peeling will stop to reveal soft, smooth feet.
Moisturizing Lotions, Creams, Gels
Choosing an effective moisturizing lotion, cream, or gel is to pick one that is extraordinarily rich and heavier than what you would use on other parts of the body.
Hard skin on foot keeps coming back?
Products that contain 40% Urea, essential oils, alpha-hydroxy acids, or those designed explicitly for callus softening or removal will help.
Since they all work well at softening, healing, and removing dead skin off feet, personal preference determines whether you choose to use a lotion, cream, or gel.
Moisturizing Socks – Wear Socks to Bed
Moisturizing socks, which contain a softening and moisturizing gel, help to repair, soften, and heal skin overnight or anytime you slide them on while relaxing.

The socks are lightweight and won’t make your feet sweat.
Any good pair of clean, cotton socks work wonders while worn overnight after slathering on moisturizing cream after a right foot soak and exfoliation.
Feet will look healthier and feel much softer after using this method.
Correction of Medical Issues – Eczema, Psoriasis and Weight Issues
Before any skin condition turns into an extremely painful or emergency, turn to a podiatrist or medical professional.
They can thoroughly assess what is going on with your feet and rule out a more serious health issue.
Common remedies for foot conditions such as eczema and psoriasis include medicated anti-fungal topical creams, in prescription strength.
Maintaining a healthy weight is important because excess weight puts extra stress and strain on your feet.
The additional weight results in swelling, dryness, and/or excessive sweating, which all lead to more trouble with your feet.

Exfoliation will make a tremendous difference with the hard skin on foot that keeps coming back and in the appearance of dead skin on feet, but there’s more.
If there’s one thing, dry feet and skin will respond positively to is hydration.
Boost skin hydration levels by drenching in vitamin-rich moisturizers, drinking lots of water, cutting back on dehydrating caffeine/alcohol, and increasing the amount of omega-3 rich foods in your diet.

Extremely interesting. I have just bought a premium electric callus shaver by Own Harmony. I have tested it out on my left foot. My heal is now very smooth rather than rough, it feels much better. I have diabetes, adrenal insufficiency and an under active thyroid. The article helps me to understand the why my feet are in this condition. Thank you very much for an educating read.